St Vincent’s haematologists use clinical trials to help blood cancer patients live longer
For blood cancer patients who have exhausted standard treatment pathways, clinical trials accessed through St Vincent’s Hospital Melbourne’s Haematology Unit can be a life-saving option.
Clinicians in the unit work with specialised nurses, laboratory haematologists and scientists, clinical trials staff and allied health professionals to study, diagnose and treat blood-related diseases.
An important focus of their work is treatment of the three types of blood cancers – leukaemia, lymphoma and multiple myeloma.
Life-changing clinical trials
Despite the significant progress that has been made in blood cancers over the past few decades, diagnosis of one of these three diseases can carry with it devastating consequences for a patient’s life expectancy.
“In the 1990s, the average survival time for multiple myeloma was about two to three years,” said Professor Hang Quach, Director of Haematology at St Vincent’s Hospital Melbourne.
“By 2000 it was five years. Currently the global average is seven years.”
Today, it is through clinical trials, where new discoveries are first put into practice, that the most advanced treatment options can be accessed.

Pictured: Professor Quach with a patient.
“People with blood cancers are now living longer than ever and I think this is achieved mainly through the fact that there has been a rapid translation of discoveries in the lab to the clinic via clinical trials,” Professor Quach said.
The results from clinical trials are often considered for regulatory approval so they can become part of the standard treatment and be made publicly available.
“Clinical trials are lifting the standard of care for people in Australia with blood cancers,” Professor Quach said.
Providing access for regional and rural patients
Not only is the clinical trials program giving patients the ability to access novel therapies that are not available as the current standard of care, but it is providing options for patients across Victoria and interstate.
St Vincent’s haematology research team has established ‘satellite sites’ where treatment can be provided at qualified regional centres. This allows patients to stay closer to home and their support networks, as well as supporting regional hospitals to offer the best possible treatments.
There are currently satellite sites at the Goulburn Valley State Hospital, Warrnambool Hospital and Launceston Base Hospital. There are plans to open another site at Townsville Base Hospital.
Equitable access also ensures costs associated with travel and accommodation are covered for patients who need to travel from across Victoria and interstate – as far as Townsville and Western Australia – to St Vincent’s Hospital Melbourne.
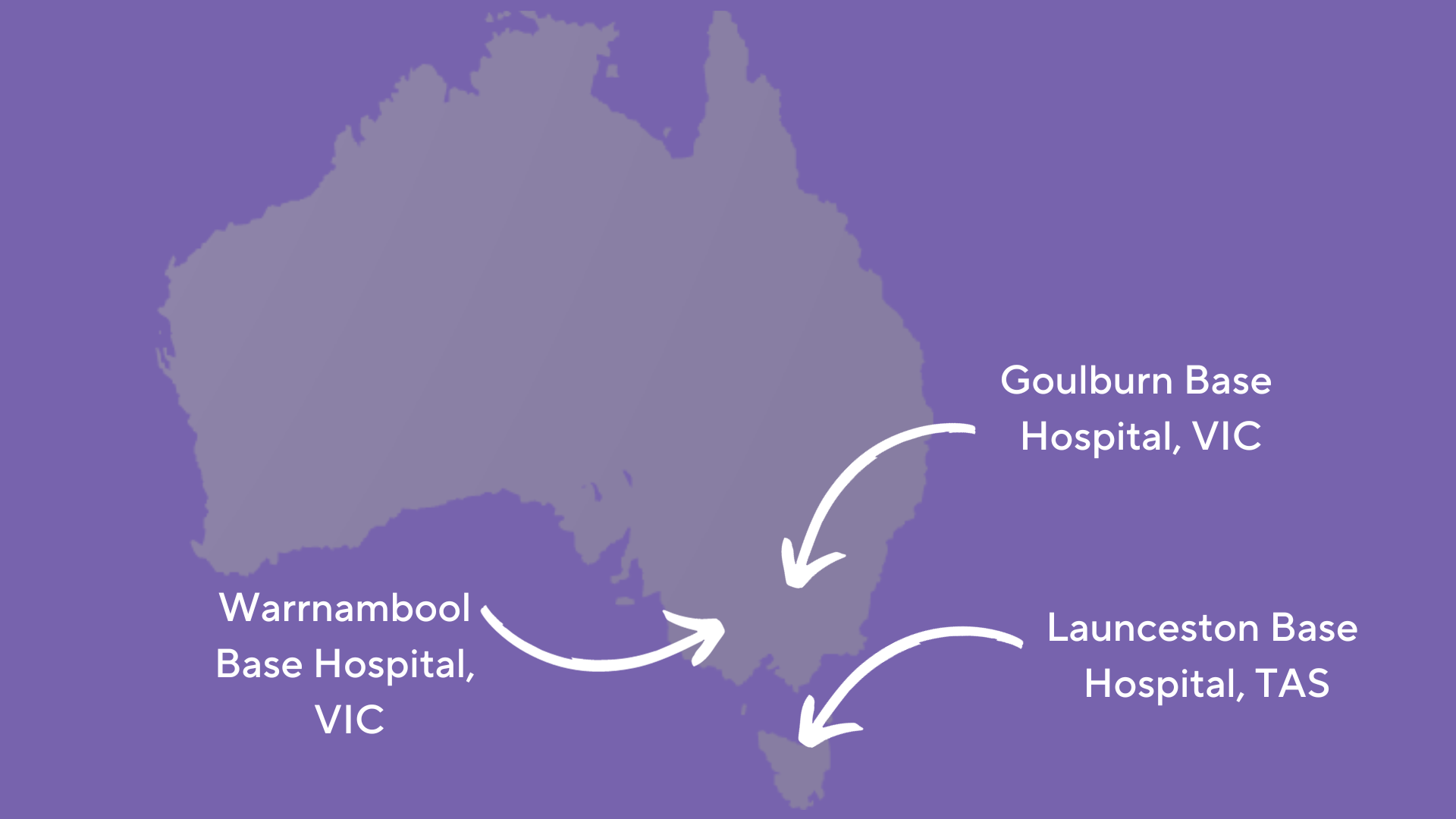
Pictured: A map of clinical trials 'satellite sites.'
Delivering a 24/7 service to achieve an operational cure
The outcomes in haematology at St Vincent’s Hospital Melbourne are the cumulative work of dozens of people across many disciplines.
There are more than 40 dedicated clinical trials staff who, since 2014, have conducted more than 210 trials and are also responsible for over 130 currently active trials.
In addition to the clinical trials staff and dedicated multiple myeloma and lymphoma nurses, there are more than 40 doctors and scientists working in laboratory haematology to provide a 24-hour service, every day of the year.
The inpatient haematology team of nurses, medical staff, allied health staff and support staff care for people with blood cancers who require monitoring and regular medical assessments in hospital.
Despite a significant proportion of blood cancers remaining incurable, Professor Quach said haematologists were optimistic about the breakthroughs that could come through continued research.
“Through new discoveries of novel agents, particularly through immune therapies, we hope to be able to utilise those therapies to keep the disease under check.”
“That would mean that even though people may not be cured, they can achieve an ‘operational cure’, which means people can live with the disease as it remains dormant for the rest of their life.”

Pictured: Some of the dozens of health professionals working in haematology at St Vincent's Hospital Melbourne.
Background on haematology
Haematology is a medical specialty that deals with blood disorders. There are two streams – clinical and laboratory haematology – which are complementary to each other.
The St Vincent’s Hospital Melbourne clinical haematology team is responsible for treating patients with blood disorders, whether a clotting or bleeding disorder or a blood cancer.
The laboratory team runs diagnostic work, including blood counts, blood clotting tests and bone marrow investigations, as well as supporting blood stem cell treatments and blood transfusions.
Laboratory haematology at St Vincent’s is headed by Associate Professor Merrole Cole-Sinclair, with Professor Quach the Director of Clinical Haematology.
While haematology as a field covers all blood disorders, cancer is a major focus due to its severity and the absence of a cure.
For more information on Haematology clinical trials recruiting through St Vincent’s Hospital Melbourne: https://www.svhm.org.au/health-professionals/specialist-clinics/h/haematology